Introduction
“Pain is the leading source of dental anxiety, it is a critical element in the dental field”.
“Pain is defined as an unpleasant sensory and emotional experience linked to real or potential tissue damage, or a sensation perceived as such damage”. Odontogenic pain is caused by a complex chain of events: tissue injury causes action potentials to be generated in the central nervous system, which is accompanied by inflammatory reactions in the affected region. Many patients are afraid of postoperative discomfort because they believe root canal treatment is the most painful type of dental treatment.
As a result, physicians will be able to predict and successfully manage postoperative pain if they have an accurate understanding of pain following root canal therapy and related factors. Furthermore, understanding the prevalence, severity, and management of postoperative pain following nonsurgical root canal therapy will reduce the need for tooth extraction and allow general practitioners to use evidence-based guidelines to manage postoperative pain.
Despite the fact that root canal treatment relieves long-term pain, postoperative pain is frequent after root canal treatment. Therefore, effective prevention and management of such pain is very much important to improve patient outcomes.
Postoperative pain prevalence and severity
During the first 24-48 hours after surgery, the incidence of postoperative discomfort ranges from 3% to 69.3%. In some investigations, mild to moderate pain was observed, while in others, moderate to severe pain was observed. Furthermore, acute postoperative pain has been recorded in some trials after 12-24 hours. The pain usually lasts for 24 to 48 hours, while some patients report that it lasts for 3 to 9 days after a root canal treatment.
Factors resulting in postoperative pain
The most prevalent cause of postoperative pain after nonsurgical root canal therapy is microorganisms, as pain is often caused by acute inflammation of the periradicular tissues. Mechanical or chemical injury to periradicular tissues is another cause of postoperative pain. Mechanical variables including over instrumentation or extrusion of root canal obturation materials have been linked to pain during endodontic procedures, while sodium hypochlorite (NaOCl) extrusion causes significant pain, edoema, and tissue injury when used as a periapical irrigant.
Factors related to postoperative pain
The presence of missed canals, periapical pathosis, inadequate cleaning and shaping, apical patency during instrumentation, apical extrusion of debris, irrigant, and intracanal medication extrusion, and overbite restorations, as well as tooth gender and type, all contribute to postoperative pain after nonsurgical root canal treatment. Preoperative and postoperative pain are linked in a significant way. Patients who are in excruciating pain prior to surgery are more likely to have severe postoperative pain.
However, the data on the link between pulpal condition and postoperative pain is mixed. Pulpal status has been linked to postoperative pain in certain studies, but pulpal status has not been linked to postoperative pain in others. During pulpitis and apical periodontitis, inflammatory mediators can cause peripheral and central sensitization, which can worsen discomfort.
Patient age was not linked to pain after nonsurgical root canal therapy in the majority of trials. Other studies, however, have found a negative link between growing age and treatment outcome in patients over the age of 35. There is no conclusive evidence that advancing age is linked to a progressive reduction of nociceptive sensitivity. As a result, changes in physiological pain systems are not linked to decreased pain sensitivity as people get older. Pulp chamber recession, on the other hand, makes root canal treatment more difficult in elderly individuals and causes more significant postoperative discomfort. Nonsurgical root canal treatment causes more discomfort in women than in males.
Gender disparities could be explained by biological differences between men and women caused by alterations in serotonin and non-adrenalin hormones. Cortisol, too, influences pain perception and is secreted in greater amounts in men than in women.
Oestrogen, the menstrual cycle, lifestyle, and societal expectations may all play a role in gender differences in pain physiological responses. In the mandibular arch and molar teeth, the incidence of pain after nonsurgical root canal therapy is considerably higher. This difference could be due to the mandibular bone’s dense trabecular structure, which reduces blood circulation.
The complicated architecture of the lower molars has similar consequences. The preservation of apical patency during root canal instrumentation has no effect on discomfort following root canal treatment. However, expansion of the apical foramen as a result of excessive instrumentation during root canal therapy may increase the frequency and severity of postoperative pain.
Number of clinic visits and postoperative pain
More than 70% of dental schools have advocated single-visit root canal therapy in the previous few decades. Endodontic innovations including nickel-titanium rotary instrumentation, trustworthy apex locators, ultrasonics, microscopic endodontics, digital radiography, improved obturation methods, and biocompatible sealing materials have made endodontic operations more efficient and enabled single-visit rather than multiple-visit root canal treatments.
However, according to certain studies, many practitioners execute root canal treatments over a number of appointments. Despite the fact that the majority of studies identified no significant differences in postoperative pain between single-visit and multiple-visit root canal procedures, the occurrence of postoperative discomfort is worrying.
However, some studies have found that single-visit root canal procedures cause more postoperative pain, contrary to assertions that single-visit root canal treatments cause less postoperative pain. These discrepancies may arise from differences in treatment techniques (such as rotary instrumentation vs. manual instrumentation or lateral condensation vs. warm vertical obturation), sample size, whether teeth are single- or multi-rooted, pulp status, and pain measurement techniques.
Pretreatment-analgesia, given 30 minutes prior to root canal treatment, lowers post-operative discomfort and may thus be beneficial, particularly in patients with low pain thresholds. Pretreatment-analgesia using nonsteroidal anti-inflammatory medicines (NSAIDs) before endodontic treatment inhibits the cyclooxygenase (COX) pathway, which may prevent pain signals from being sent to the brain. Furthermore, a single oral dosage of prednisolone (30 mg) or dexamethasone (4 mg) given before surgery significantly lowers postoperative discomfort. The use of a long-lasting local anesthetic (bupivacaine) during therapy can also help.
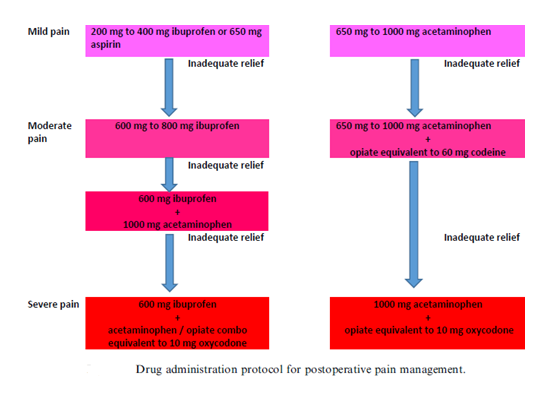
Courtsey: J Taibah Univ Med Sci. 2017 Oct; 12(5): 376–384.